Virtual physiotherapy is an evidenced-based assessment and treatment method that can be delivered through video or telephone consultation.
Whilst it cannot replace all face-to-face interaction, it is an effective and appropriate method of care for the majority of non-complex musculoskeletal conditions and the assessment and ongoing treatment of these.
Virtual physiotherapy covers a range of services, with best practice solutions including:
- Digital triage - patients answer a series of questions online and intelligent software helps to determine the most appropriate care pathway to meet the needs of the patient
- Remote consultations - physiotherapists deliver videocall consultations using technology that enables exercise videos, advice and education, and patient records to be accessed during the appointment
- Self-management - advice, education and digital exercise prescriptions are accessed by the patient at their convenience through an app that supports video content, progress trackers and other tools that encourage education and engagement
When many people think of physiotherapy they think of manual therapy, but while this is an important part of a clinician’s work it is only one element. Clinicians can use virtual physiotherapy to provide education and advice to help patients manage and improve their symptoms. They can also guide patients with self-management and progression support techniques, including exercise therapy and rehabilitation, self-joint mobilisation, self-trigger point release and other soft-tissue treatments and functional movement re-education strategies. Clinicians can also advise on the purchase of appropriate home exercise equipment and other off-the-shelf devices which may support recovery, such as wrist splints or supports.
Until fairly recently, virtual physiotherapy services represented the minority of support offered by both the private and public healthcare sectors. This was until the Covid-19 crisis created a sudden need for digital services to be rolled out more widely across the industry.
This report aims to deliver best practice advice for the industry based on more than 12 months of virtual physiotherapy treatments administered through an award-winning app. The findings are informed by data from 27,000+ patients, learnings from virtual physiotherapy expert clinicians and feedback from patients that have been through the process.
The impact of Covid-19 on physical injuries and digital health
The Covid-19 outbreak and resulting UK lockdown put a halt to in-clinic rehabilitation treatment for thousands of patients. Prior studies that map treatment adherence against outcomes¹ suggest that this break in treatment could have a huge impact on long-term outcomes for patients who didn’t access alternative support.
The unique set of circumstances created by the crisis also increased the chances of many people developing new injuries, further enhancing the need for physiotherapy services. Publications aimed at runners warned of the perils of many people upping their mileage too quickly², a study in the Bone and Joint Journal reported a 26% rise in the number of DIY-related hand injuries³, the British Orthopaedic Association reported a rise in trampoline injuries⁴ and research by Ascenti showed that home-working from the sofa for sustained periods had left half the workforce in pain⁵.
Providing further evidence of the impact of this, Google Trends data⁶ shows that in the eight weeks following the lockdown being introduced on 23 March, there was a 102% jump in searches for advice on knee pain, a 91% rise in searches for sprained ankle content and an 86% increase in the number of searches for articles on shin splints.
As lockdown measures ease, at the time of writing there are also concerns about how deconditioning could cause a new spike in injuries. The NIHR Nottingham Biomedical Centre said increases in sedentary activity will have impacted metabolic function and muscle volume, particularly for older people⁷, a number of athletes have cautioned about the injury risks of rushing back to competitive sport too quickly⁸,⁹ and the British Society of Rehabilitation Medicine has warned that those recovering from Covid-19 will have experienced severe deconditioning¹⁰, which could increase their chances of injury.
In this environment, The Lancet reported that telemedicine is being embraced ‘like never before’¹¹, while a webinar by the Healthcare Information and Management Systems Society (HIMSS) predicted that the growth in adoption of digital health services will continue post Covid-19¹².
Comparing the results of virtual and in-person treatment
Background
As a world-leading provider of virtual physiotherapy, with an award-winning digital service that has been in operation for 12 months, Ascenti wanted to use its data to explore how the results of online care compare with in-person support.
A comparative observational study was conducted using data collected from routine care provided by qualified Ascenti physiotherapy practitioners. Patients involved in the study were referred to Ascenti for a range of needs.
The study involved exporting anonymised data that mapped the treatment journeys of 27,096 patients who had accessed virtual physiotherapy support before and during the Covid-19 crisis - running up until 10 June 2020. Of this population, 9,506 had received virtual-only treatment, while 17,590 had received a mix of virtual and face-to-face care.
A control group was then built using the data of 6,226 patients who had been treated with in-person physiotherapy only.
Interventions
The study compared three options:
- Virtual physiotherapy only - all treatment sessions delivered via videocall using the Ascenti Physio app, which also enables patients and clinicians to access videos and patient records within the call and afterwards at their convenience
- Face-to-face physiotherapy only - all treatment sessions delivered in one of Ascenti’s 300 community clinics. Treatment could include manual therapy as well as exercise prescriptions and advice, all delivered in-person. This treatment did not include access to the Ascenti Physio app
- Integrated virtual and face-to-face physio support - a mixture of face-to-face and virtual physiotherapy treatment, including at least one visit to a community-based clinic and full access to online appointments and tools through the Ascenti Physio app
Results
The analysis revealed that patients are open to trying virtual physio when it is recommended to them. Upon the closure of Ascenti clinics due to Covid-19, 81% of patients agreed to have virtual sessions and continued with them beyond their first session.
Measured on a 10-point pain Numerical Rating Scale (NRS) all patient groups saw significant reductions in their levels of pain following treatment, regardless of what type of treatment they accessed and regardless of the severity of their injury or condition.
In the population-level analysis, patients that combined face-to-face treatment with virtual sessions delivered through the app saw the biggest improvements, moving from a 5.4 NRS score at initial assessment to 1.8 at discharge - an improvement of 3.6 points on average. Patients who only accessed face-to-face treatment reduced their pain by 3.4 points on average, while people who were treated virtually and didn’t see a physio in-person improved by an average of 3.1 points.
Further analysis was then conducted to explore how virtual appointments compared with in-person physio when treating different pain levels. The study found that for patients whose NRS score was low or medium, the difference in results between virtual and face-to-face interaction was negligible. Patients with a low NRS score at initial assessment saw an improvement of 1.5 from virtual treatment compared to 1.6 from face-to-face, while patients with a medium NRS score improved by 3.5 with virtual physio compared to 3.6 with face-to-face.
As might be expected, the study found that the difference in outcome between virtual and in-person treatment was more pronounced for patients that scored high on the NRS scale at initial assessment. However, while those patients who only accessed face-to-face treatment did see a 5.2 point improvement, those who were treated virtually still saw a substantial 4.7 point improvement without any manual therapy. This suggests that, even for more severe injuries or conditions, digital treatment remains a viable alternative to in-person physio, while the best results for this group - and overall - were enjoyed by patients that accessed integrated support.
One additional finding from this data supports the idea that engagement in exercises improves outcomes, over-and-above any manual treatment and face-to-face interaction. Patients whose anonymised records showed they accessed exercise videos through the app as part of their virtual treatment saw the biggest improvements in every severity category (low, medium and high NRS). Overall though, integrated support still achieved the best results, perhaps because a greater proportion of patients with high NRS scores were treated with this method.
A final and important finding is that the data suggests that patients who access virtual physiotherapy services are happy with the results. Survey data showed that 92% of patients who were treated virtually were satisfied with its effectiveness and 77% would be ‘extremely likely’ to recommend the service to friends and family. While this is slightly lower than the results for face-to-face treatment, which were 97% and 81% respectively, it is likely that the gap will close further as trust in virtual physiotherapy increases.
Limitations
It is important to note some of the natural limitations of this study. This study is based on the experiences of patients referred for physiotherapy treatment for a range of needs. Some of the conditions were gradual onset, while others were traumatic. The results must therefore be interpreted as general findings and it should not be assumed that they apply equally to all injury types - for example those involved in Road Traffic Accidents.
In addition, many of the patients that fall into the integrated treatment category were being seen face-to-face before the Covid-19 lockdown and in some cases their virtual treatment was just for their last one or two sessions. Finally, some of the patients that did not transition to virtual treatment may have had more severe conditions that would have responded less well to remote treatment. It is likely that these factors will have had some influence on the clinical outcomes recorded in this data, however, it is felt that it wouldn’t have significantly changed the overall picture.
Further research
It would be beneficial to conduct further research that is targeted at measuring the results of
virtual physiotherapy on different injury types, for example Road Traffic Accident trauma cases or more serious sports injuries.
It could also be useful to explore whether the convenience of virtual treatment increases the likelihood of people seeking support for their conditions and whether it increases people’s adherence to an ongoing programme of rehabilitation.
The advantages and disadvantages of virtual physiotherapy
Advantages
Supporting patients with their physiotherapy needs through a virtual service holds a number of advantages over in-person care. These include:
- Convenience - Patients are often delighted to be able to access treatment from the comfort of their own home. It saves them an enormous amount of time as they only need to set aside 30 minutes for the appointment itself rather than account for travel time and there is no need to arrange childcare, transport or book time off work. The convenience of this may make them seek early treatment and maintain a course of treatment for longer, as appointments will be less disruptive to their lives.
- Patient-centred treatment - While patients attending an in-clinic appointment often expect hands-on treatment, virtual physiotherapy enables a more holistic patient-centred focus. The format encourages more conversation and provides the clinician with a better opportunity to ask questions and provide bespoke advice, education and reassurance, while also tackling some of the psychosocial aspects of pain. Some clinicians can really excel in this area.
- Patient engagement - due to not being able to receive manual therapy in a virtual appointment, many patients recognise that the onus is on them to use the sessions to take control of their own rehabilitation. This approach encourages accountability and can be very motivating for the right patient as they become more engaged in the information and advice they are given.
- Insight into home situation - a virtual appointment enables the clinician to gain a better understanding of the patient’s home environment. They see what home exercise equipment they can access and what space they have available, and they may get a chance to review things like their home-working set-up, which could be useful if that has contributed to their injury. These kinds of insights, which aren't available in a typical in-clinic appointment, can enable physios to provide bespoke advice that is more tailored to their circumstances.
- Digital tools - best practice virtual physiotherapy doesn’t stop with a videocall appointment; rather, innovative digital health platforms like the Ascenti Physio app can provide patients with access to a range of tools. These include demonstration videos, goal-setting facilities and progress trackers, which can all be accessed inside the appointment and afterwards. These tools can also provide notifications and reminders to encourage greater adherence to prescribed exercises.
- Appropriate referrals - digital triage removes the strain of inappropriate referrals on healthcare services by directing patients towards services that best meet their needs. This avoids wasted time for both clinicians and patients and improves cost-effectiveness, while ensuring that capacity is used appropriately.
The disadvantages of virtual physiotherapy
- Missing the power of therapeutic touch - this can be an important point from both the patient’s and the therapist’s perspective. Manual assessment and treatment can provide the opportunity for the clinician to feel different tissues, tension, spasm, and depth of symptoms, which is necessary in some cases and cannot be recreated virtually. There are times too when patients report that they feel they need someone to press, stretch and release areas that they just can’t reach through home exercises. Being in the same physical space as a patient also gives clinicians the opportunity to use their hands to correct movement and exercises to help patients to follow them correctly. The use of touch to demonstrate empathy or offer support at times of distress or upset, which can be an important part of compassionate care, is also missing.
- Lack of opportunity for diagnostic tests - there are a number of diagnostic tests that physiotherapists can use to aid their decision-making and screen for problems such as neurological loss. Some of these tests can’t be modified for a virtual call and so this could leave a gap in clinical reasoning that could reduce effectiveness in some cases and, in a small number of cases, could lead to safety issues.
- Reduced trust for some patients - some patients may be more likely to trust a diagnosis that is given to them after a physical examination. This could be partly because they don’t feel confident in their own ability to describe their pain and symptoms or it could be because virtual physiotherapy is still relatively new. Certain situations, for example asking a patient to undress or uncover an area for examination, can also feel more awkward over video than in-person.
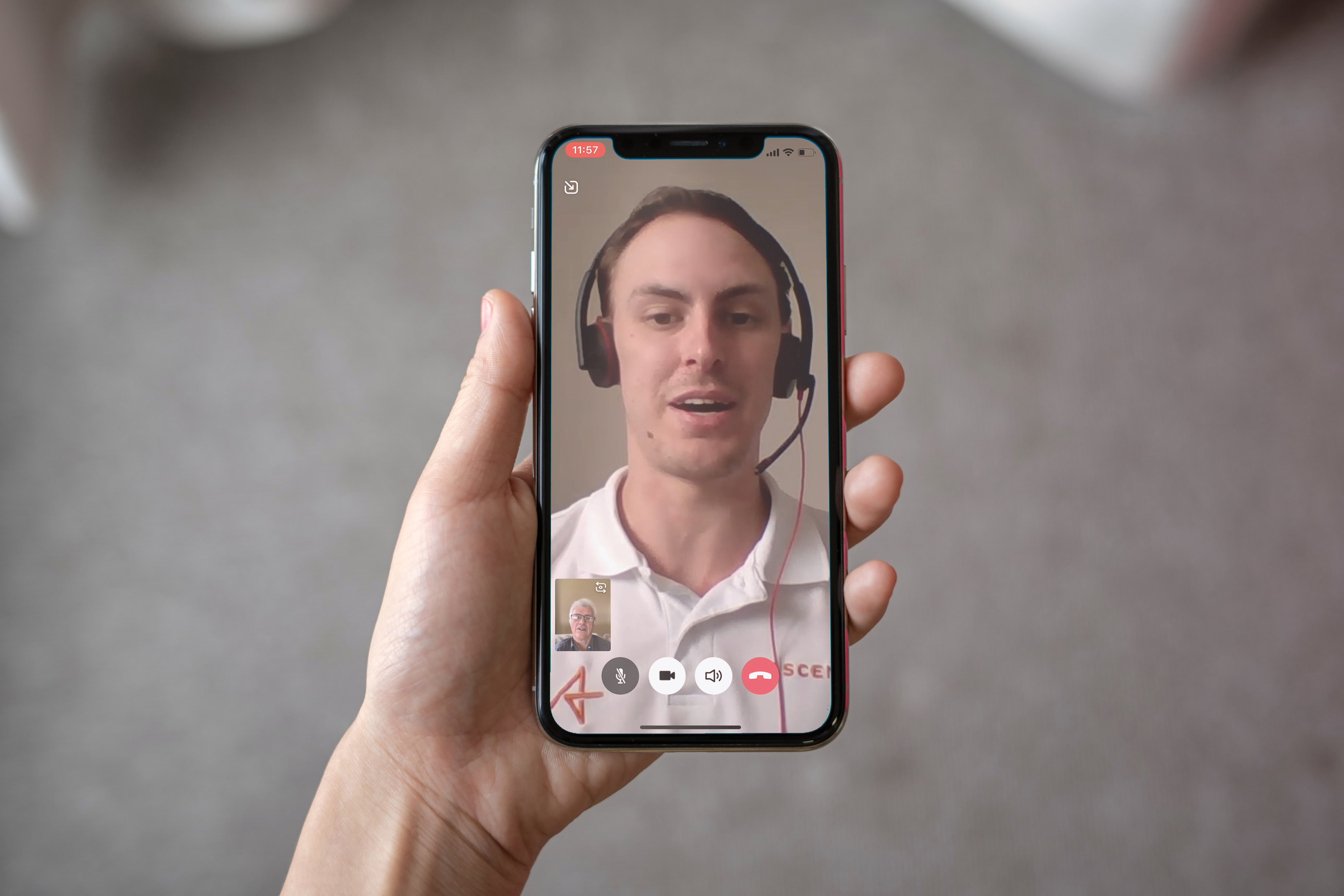
The future for virtual physiotherapy
With a Covid-19 vaccine not expected to be available until 2021¹³ and many people likely to want to minimise their risk of infection until then, it is likely that the need for digital healthcare services will remain high in the short-to-medium term.
This will provide the opportunity for clinicians and technologists to add new innovations, strengthen their evidence base and support more patients using this emerging treatment option. All of these things will help establish a greater trust in virtual physiotherapy.
As we eventually move past Covid-19, familiar barriers to in-clinic treatment will re-emerge to front-of-mind, with patients putting off accessing support due to lack of time, family commitments and the inability to travel. It is likely that virtual physiotherapy will become an increasingly attractive option for people in these circumstances.
The results of this study - potentially the world’s largest study of virtual physiotherapy conducted so far - demonstrate that patients who access digital support to help them with MSK injuries can achieve excellent results.
While there are some treatments and diagnostic tests that can’t be modified to be delivered virtually there are huge benefits in convenience, patient engagement and patient insight that can help make up for that. Even more excitingly, digital leaders are creating innovative apps that support education, motivation and behaviour change inside the videocall and outside it too, available to be accessed 24/7.
Key to the success of virtual physiotherapy going forward will be the ability of healthcare providers to identify the circumstances when this treatment should be offered; providing the right treatment, at the right time, to the right patient through the right clinician.
- Right treatment - virtual physiotherapy isn’t the best way to treat all conditions and healthcare providers will need to know when in-person treatment might be a better option, and when there simply isn’t an alternative to manual therapy as part of their care.
- Right time - in many cases the best journey for a patient will be a combination of virtual and in-person treatment, and it will be up to the healthcare provider to understand when to offer each in order to best treat the condition and achieve the best adherence from the patient.
- Right patient - some patients will be more motivated by the extra accountability of virtual physiotherapy and more confident in using the technology, while others will be more comfortable with - and therefore see better outcomes from - traditional in-clinic sessions. Healthcare providers must become adept at recognising what will get the best results for each particular patient.
- Right clinician - virtual physiotherapy is, in many ways, a very different discipline. Some clinicians are experts at winning patient engagement, picking up on signals in body language or the home environment and using technology to its full advantage, while others truly excel in an in-person environment and in delivering manual therapy. Healthcare providers should ensure they deploy their clinical talent most effectively.
The results of this study of 27,000+ patients shows that, in many cases, online and video physiotherapy treatment can achieve the same strong outcomes as in-clinic, as long as this treatment is delivered effectively by digitally trained physiotherapists using purpose-built technology and accessed by patients who are empowered to take a greater role in their own rehabilitation.
For patients with more severe injuries it is likely that in-person treatment will be needed for them to achieve a full recovery, but virtual therapy can still be a part of their journey too and can make regular appointments and check-ups easier and more convenient.
Ultimately, it appears that the very best results are achieved when patients benefit from a mixture of innovative digital care and elite-quality in-person treatment to support them through the different stages of their treatment journey. Deployed together, this combination can help raise standards in the profession and enhance physiotherapy results overall.

About Ascenti
Ascenti is the leading independent provider of physiotherapy and selected clinical outsourcing services in the UK. It is a trusted partner to more than 20 NHS Clinical Commissioning Groups (CCGs) and 400 private businesses across the UK, serving NHS patients, pay as you go customers and private medical insurance members.
With extensive national coverage, Ascenti has over 300 highly trained physiotherapists delivering upwards of 600,000 treatment sessions annually. Enabling people to make headway after illness and injury, step back in to work after accidents, or simply stay active and keep moving forward in their daily lives.
Ascenti is a dynamic and progressive company – advancing physical therapies by making them more accessible to all, raising standards and pioneering new digitally enabled physiotherapy and musculoskeletal (MSK) services through its ISO-accredited workflow platform and award-winning app, which provides 24/7 access to expert advice through digital triage, virtual consultations and tailored exercise programmes.
Top physiotherapists and elite sportsmen and women helped found Ascenti and continue to lead it today, constantly shaping and improving its clinical approach. Ascenti physiotherapists are employed by the organisation and every clinician undertakes a minimum of 100 hours of protected training and CPD time annually as part of the company’s award-winning Clinical Development Programme. This helps Ascenti to maintain consistently high standards of governance and keeps them at the cutting edge of the latest technologies and treatments.
References
1. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2923776/
2. https://www.runnersworld.com/uk/health/injury/a30281450/avoid-running-injuries/
3. https://online.boneandjoint.org.uk/doi/full/10.1302/2046-3758.15.BJO-2020-0028.R1
4. https://www.boa.ac.uk/policy-engagement/journal-of-trauma-orthopaedics/journal-of-trauma-orthopaedics-and-coronavirus/the-paediatric-trauma-burden-of-uk-lockdown-early.html
5. https://www.ascenti.co.uk/news-article/home-workers-report
6. https://trends.google.com/trends/explore?date=2020-03-23%202020-06-15&geo=GB&q=knee%20pain,sprained%20ankle,shin%20splints
7. https://nottinghambrc.nihr.ac.uk/about-nottingham-brc/news/533-inactivity-due-to-covid-19-lockdown-measures-can-greatly-worsen-health-problems-say-international-researchers
8. https://www.telegraph.co.uk/athletics/2020/05/25/athletes-should-write-year-rather-risk-injury-says-kelly-sotherton/
9. https://www.independent.co.uk/sport/football/premier-league/coronavirus-premier-league-kevin-de-bruyne-manchester-city-news-a9444091.html
10. https://www.bsrm.org.uk/downloads/covid-19bsrmissue1-published-27-4-2020.pdf
11. https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(20)30818-7/fulltext
12. https://www.himsslearn.org/accelerating-health-systems%E2%80%99-digital-transformation-why-digital-health-must-be-new-standard-post
13. https://www.healthline.com/health-news/heres-exactly-where-were-at-with-vaccines-and-treatments-for-covid-19#Vaccines
